Clinical Applications
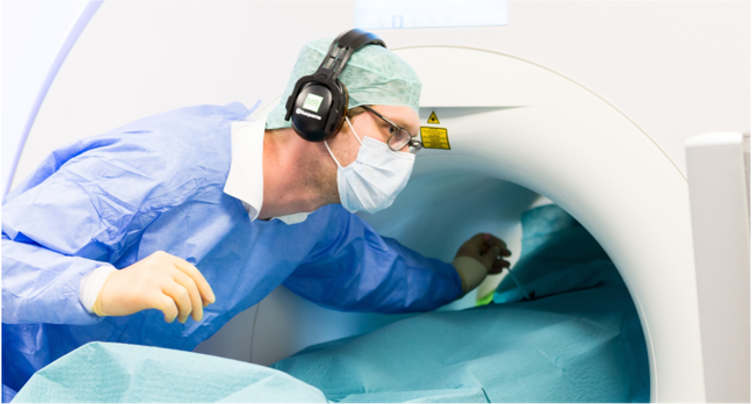
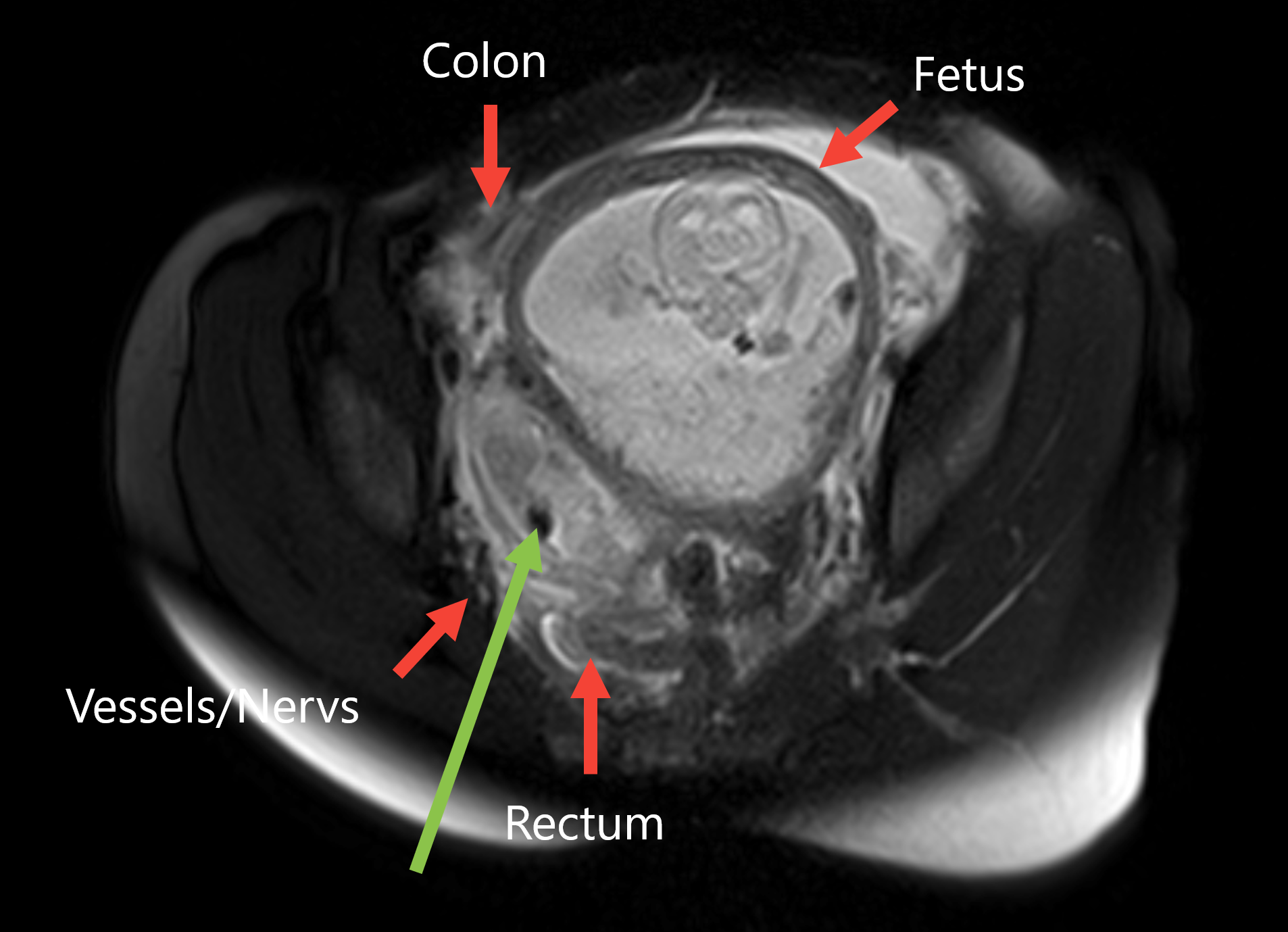
MRI (Magnetic Resonance Imaging) offers a multitude of advantages that have established it as a pivotal tool in modern medicine. Firstly, MRI is a non-invasive imaging technique, eliminating the need for harmful ionizing radiation present in other imaging methods. This makes it safe for patients of all ages, including children and pregnant women. Additionally, MRI provides exceptional soft tissue contrast, allowing for the clear visualization of various structures within the body, including the brain, spinal cord, organs, and joints. Its high-resolution images aid in the early detection and accurate diagnosis of a wide range of conditions. With its exceptional capabilities, MRI continues to play an integral role in advancing medical knowledge, guiding treatment decisions, and enhancing patient care.
Our group uses MRI for different types of interventions, such as:
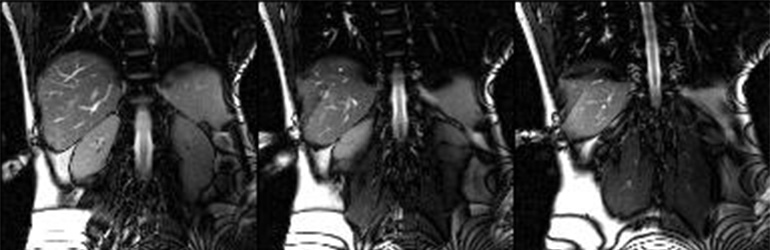
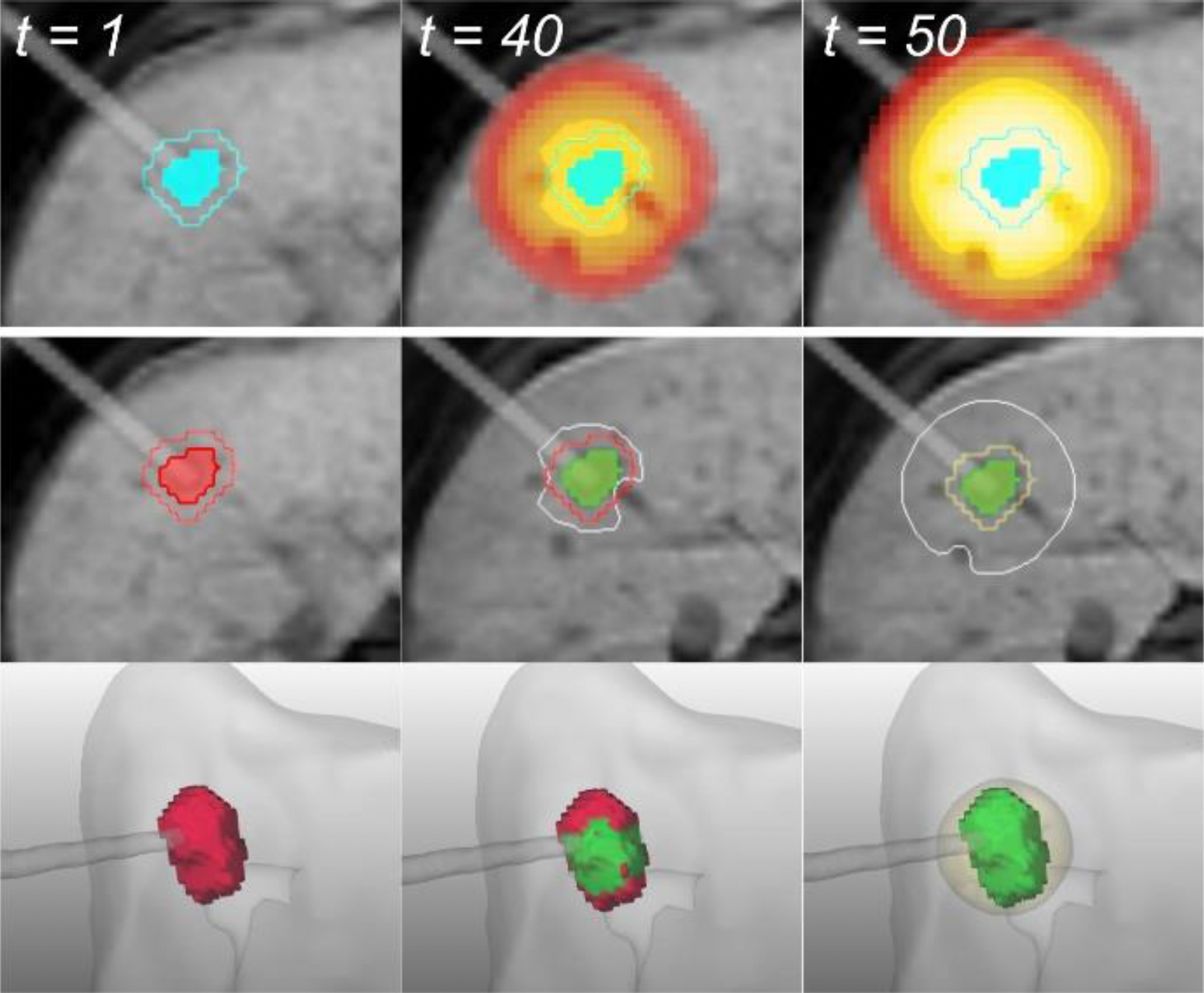
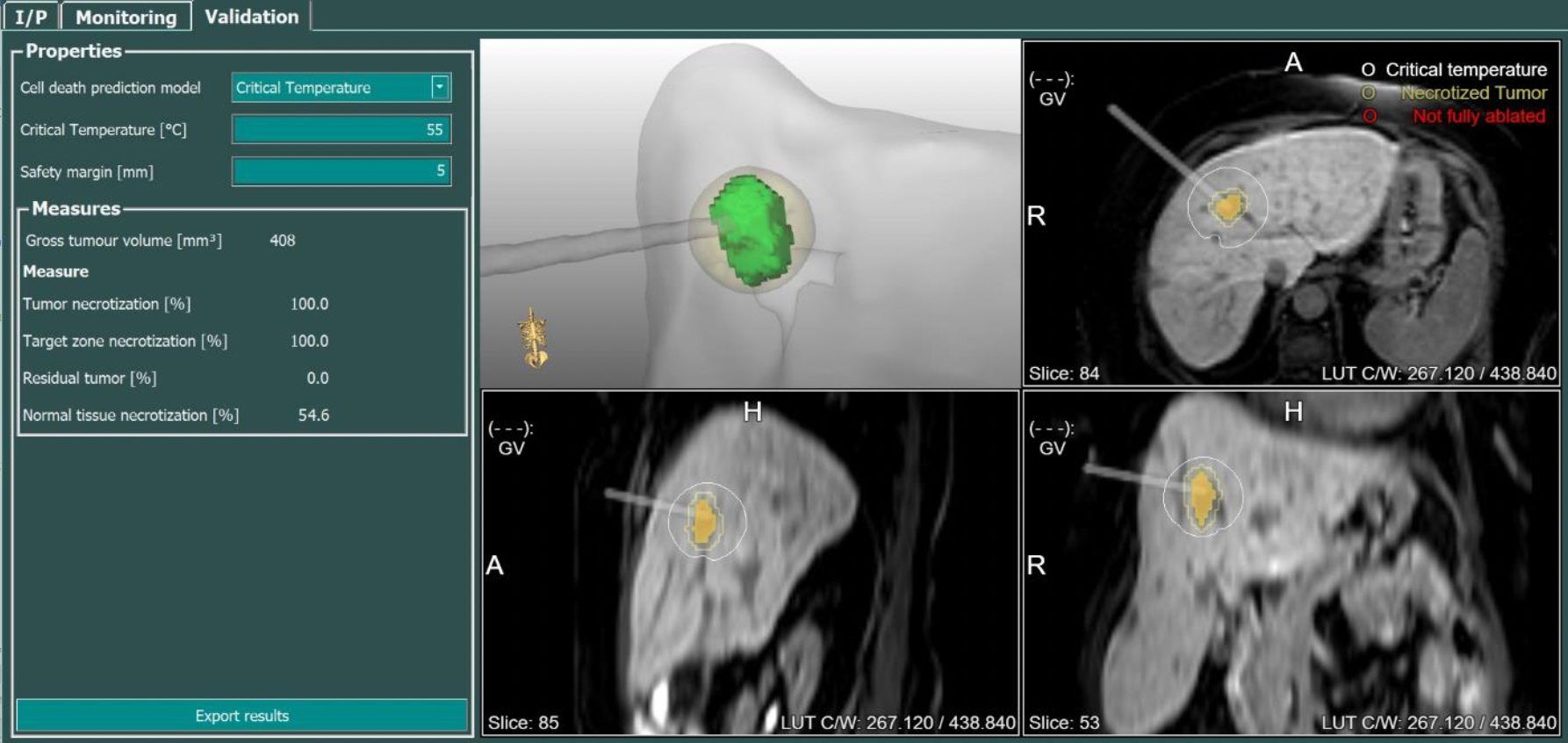
MR-guided percutaneous ablations involve using real-time Magnetic Resonance Imaging (MRI) guidance to perform minimally invasive procedures that destroy or remove abnormal tissue. This technique allows for precise targeting of the tissue to be ablated, such as tumors or lesions, while minimizing damage to surrounding healthy tissue. During the procedure, the MRI scanner provides detailed images that help guide the placement of needles or probes into the target area (Fig. 1). Once positioned, energy, such as microwaves, radiofrequency or laser, is delivered through the needles or probes to heat or destroy the abnormal tissue. Progress of the procedure is monitored by MR-thermometry with so called temperature maps. These maps allow accurate temperature measurements and can be used to predict the destroyed volume ensuring good treatment outcomes (Fig. 2, 3).
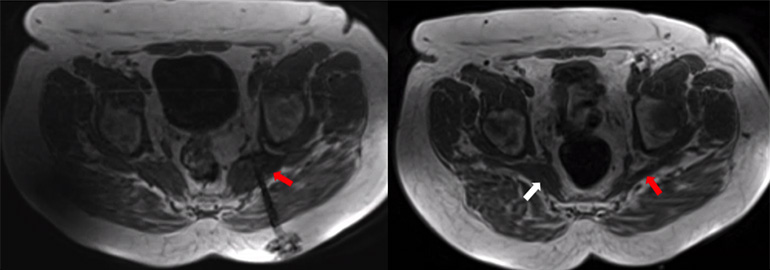
MR-guided pain therapy for piriformis pain syndrome utilizes real-time MRI to guide the precise placement of therapeutic interventions. This technique involves visualizing the affected area, such as the piriformis muscle and the impinged sciatic nerve, using MRI. The MRI images help identify the location and severity of the condition, enabling accurate diagnosis and treatment planning. Therapeutic interventions, such as targeted injections of medication, are then administered under MRI guidance. This approach improves the accuracy of treatment delivery, minimizes the risk of complications, and enhances pain relief for individuals with piriformis pain syndrome.
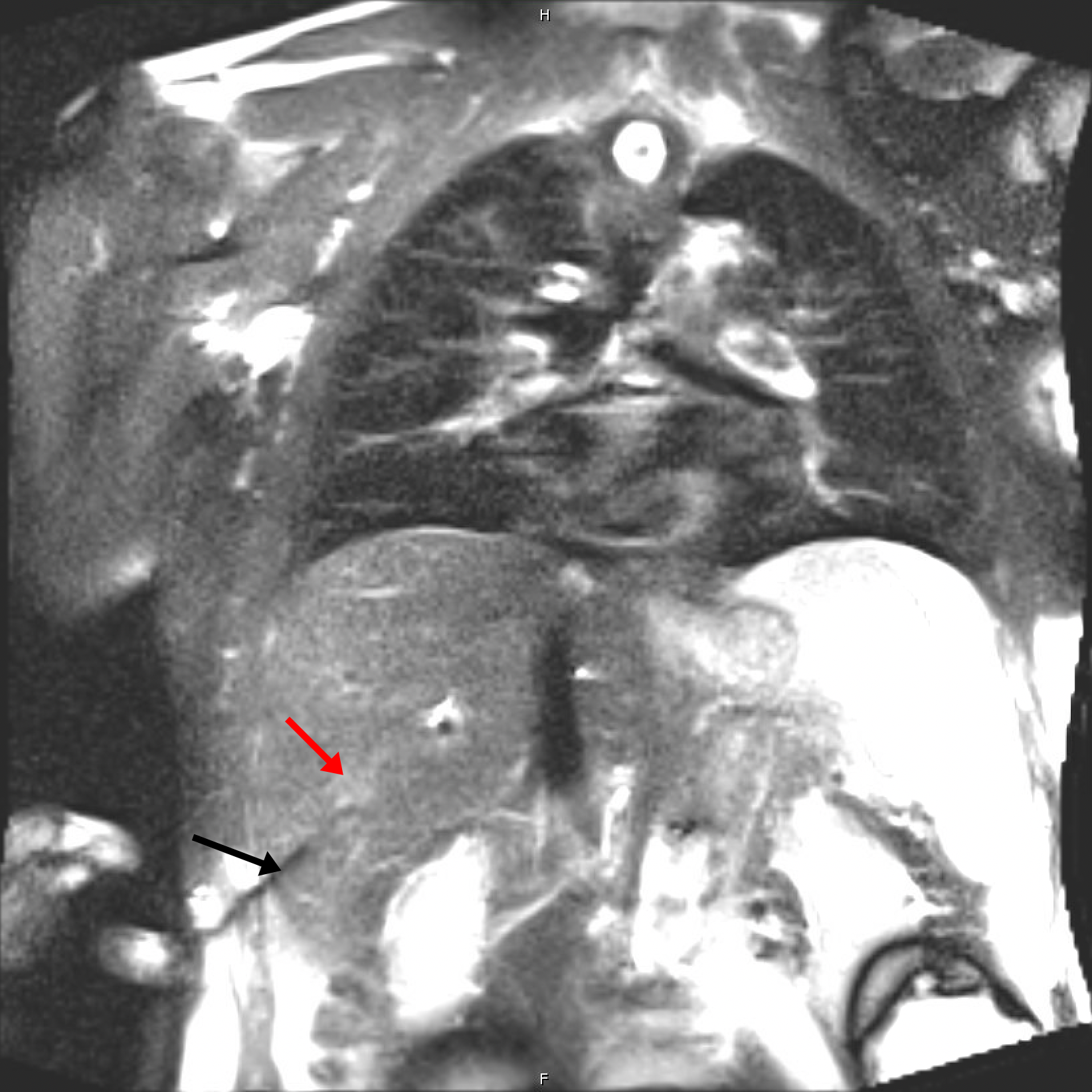
MR-guided biopsy is a minimally invasive medical procedure that utilizes magnetic resonance imaging (MRI) technology to guide the precise sampling of tissue from within the body. This advanced technique is commonly employed in the diagnosis and assessment of various medical conditions, particularly in the detection of suspicious or hard-to-reach lesions, tumors, or abnormalities. MR-guided biopsies offer the advantage of including real-time visualization of the target area. This approach is especially valuable in oncology, as it aids in obtaining representative tissue samples for accurate diagnosis and treatment planning, ultimately contributing to better patient care and outcomes. Below you can see a typical case for a MR-guided biopsy on the liver where the needle is inserted into the tumor tissue (Fig. 5).
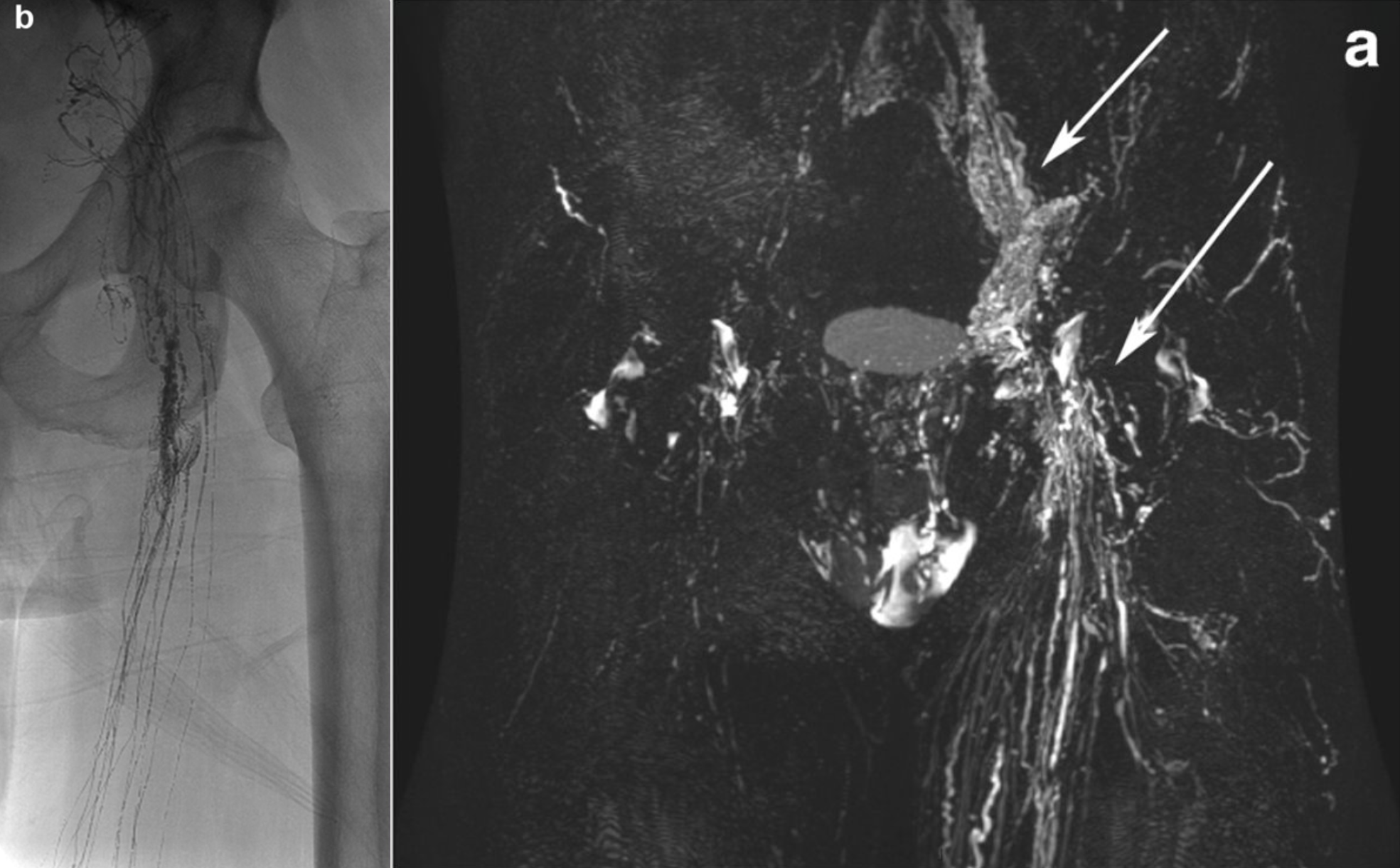
The lymphatic system transports tissue fluid, fats, and immune cells. Disorders can cause lymph leakage or drainage problems, leading to conditions such as chylothorax, lymphatic fistulas, or persistent fluid collections. Lymphangiography is a minimally invasive imaging technique in which contrast agent is injected into lymph vessels (usually in the foot or groin) to visualize the lymphatic system and detect leaks using MRI. It also enables treatment: leaking vessels can be sealed and abnormal connections corrected, often avoiding surgery. Our group uses lymphangiography for both precise diagnosis and minimally invasive therapy, allowing targeted treatment even of very small lymph vessels. Below you can see a the lymphatic system in the pelvis of a patient and the leakage causing lymph to exit (Fig. 6).
An abscess is a localized collection of pus caused by infection, which can occur in the abdomen, organs, or soft tissue and lead to pain, fever, and general deterioration. Percutaneous abscess drainage is a minimally invasive treatment in which a thin catheter is inserted into the abscess under imaging guidance (ultrasound, CT, or MRI). This allows continuous drainage of pus, relieving pressure and promoting healing. The technique enables precise catheter placement while minimizing damage to surrounding tissue and often avoids major surgery. It is typically combined with antibiotic therapy. In our group, abscess drainages are routinely performed using modern image guidance, helping patients recover faster and reducing hospital stays.